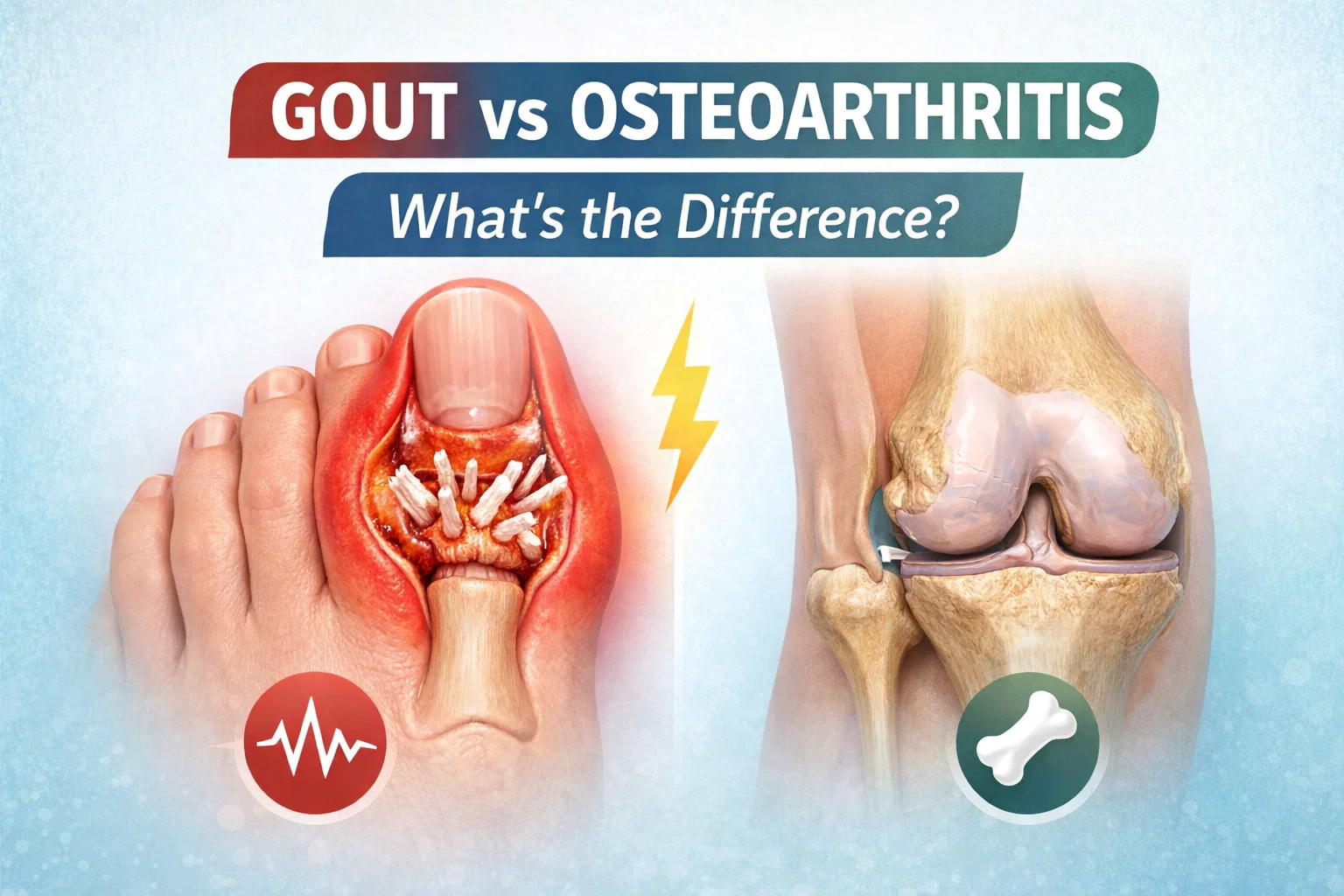
Gout vs Osteoarthritis Symptoms, Causes, and Key Differences Infographic
Understanding the difference between various types of joint pain can be the turning point in your journey toward long term wellness. When you wake up with a throbbing toe or a stiff knee, your mind immediately searches for answers. Is it just the wear and tear of a busy life, or is there an internal chemical imbalance at play? The image of Gout versus Osteoarthritis provides a stark visual representation of two very different conditions that both fall under the umbrella of arthritis. While they both cause discomfort and limit mobility, their origins, symptoms, and treatments are worlds apart. In this guide, we will dive deep into the mechanics of these conditions to help you navigate your health with confidence and clarity.
Defining the Core Differences: Inflammation vs. Degeneration
To truly grasp what is happening inside your joints, we have to look at the underlying biological processes. Gout is fundamentally an acute inflammatory arthritis. It is caused by the accumulation of urate crystals within the joint space. These crystals are needle-like and sharp, which explains why a gout attack feels so sudden and agonizing. It is essentially a metabolic issue where the body either produces too much uric acid or the kidneys fail to excrete it efficiently.
On the other hand, Osteoarthritis is classified as a degenerative joint disease. Think of it as the protective buffering system of your joints slowly wearing down over time. It is not caused by a sudden chemical spike but rather by the mechanical breakdown of cartilage, which is the firm, slippery tissue that cushions the ends of your bones. When this cartilage thins, the bones begin to rub against each other, leading to structural changes that develop over years rather than hours.
Shutterstock
The Visual Indicators of Gout
In the visual comparison, Gout is often depicted affecting the big toe, a condition known as podagra. You can see the intense redness and swelling that characterizes an attack. Inside the joint, the presence of urate crystals creates a high friction environment that triggers a massive immune response. This leads to the classic four signs of inflammation: heat, redness, swelling, and intense pain. Because it is systemic, Gout can also lead to the formation of tophi, which are visible lumps of crystals under the skin if the condition is left unmanaged for a long time.
The Structural Changes in Osteoarthritis
Looking at the knee joint in the Osteoarthritis illustration, the focus shifts to bone and cartilage. You will notice cartilage thinning and joint space narrowing. As the body attempts to compensate for the loss of cushioning, it often grows extra bits of bone at the edges of the joint. These are called osteophytes, or bone spurs. These spurs can cause a grating sensation known as crepitus and contribute to the visible enlargement of joints, particularly in the fingers or knees.
Symptoms and Onset: How to Spot the Signs
One of the easiest ways to tell these two apart is by looking at the clock. The timing of your pain tells a story that your doctor will find incredibly useful for a diagnosis. Let us break down how these symptoms manifest in daily life.
- Speed of Onset: Gout typically strikes like a lightning bolt, often in the middle of the night. You might go to bed feeling fine and wake up unable to bear the weight of a bedsheet on your toe. Osteoarthritis is a slow burner. The stiffness and aching creep up on you over months or years, usually becoming more noticeable after repetitive use of the joint.
- Pain Quality: Gout pain is often described as excruciating, burning, or throbbing. Osteoarthritis pain tends to be a deep, dull ache that worsens with activity and improves with rest, though morning stiffness is a common complaint.
- Physical Appearance: A gouty joint is usually bright red and feels hot to the touch. An osteoarthritic joint might look swollen due to bone spurs or fluid buildup, but it rarely exhibits the intense heat and redness of an inflammatory flare.
The Role of Uric Acid and Diet
Uric acid is the primary villain in the story of Gout. It is a waste product created when the body breaks down purines, which are found naturally in your body and in certain foods. When levels get too high, the blood becomes saturated, and the acid crystallizes in the joints. This is why diet plays such a massive role in managing Gout. Foods high in purines, such as red meat, organ meats, and certain types of seafood, can trigger a flare. Alcohol, particularly beer, and sugary drinks high in fructose are also major contributors.
For Osteoarthritis, the focus is less on specific chemicals and more on mechanical load and systemic health. While diet still matters, it is more about maintaining a healthy weight to reduce the physical pressure on weight bearing joints like the hips and knees. Inflammation does play a small role in Osteoarthritis, so an anti inflammatory diet rich in Omega 3 fatty acids can be beneficial, but it is not the primary driver of the disease in the way purines drive Gout.
Managing the Flare: Immediate and Long Term Strategies
Treatment paths for these conditions diverge significantly because their causes are so different. If you are dealing with Gout, the goal is twofold: stop the current inflammation and lower your uric acid levels to prevent future attacks. This often involves medications like colchicine or NSAIDs for the short term, and lifestyle changes or urate lowering therapies for the long term.
Managing Osteoarthritis is all about preserving function and reducing pain. Since the cartilage cannot easily be replaced, the focus is on strengthening the muscles around the joint to provide better support. Physical therapy is a cornerstone of OA management. Weight loss is also incredibly effective, as losing even a few pounds can significantly decrease the force exerted on your knees with every step you take.
Quick Comparison Table for Joint Health
| Feature | Gout | Osteoarthritis |
|---|---|---|
| Primary Cause | Urate crystal buildup | Cartilage wear and tear |
| Common Location | Big toe, ankles, knees | Knees, hips, fingers, spine |
| Pain Level | Severe and sudden | Aching and gradual |
| Risk Factors | Diet, genetics, alcohol | Age, obesity, past injuries |
Why Professional Diagnosis is Essential
It is tempting to self diagnose based on an image or a quick search, but joint health is complex. Sometimes, these conditions can coexist. A person might have Osteoarthritis in their knee and then experience a Gout flare in that same joint. Doctors use a variety of tools to get the full picture. For Gout, they might perform a joint fluid aspiration to look for crystals under a microscope or order a blood test to check uric acid levels. For Osteoarthritis, X rays are the gold standard because they clearly show joint space narrowing and bone spurs.
Getting the right diagnosis early can prevent permanent joint damage. Untreated Gout can lead to joint deformity and kidney stones. Unmanaged Osteoarthritis can lead to a loss of independence and the eventual need for joint replacement surgery. By being proactive and understanding the nuances shown in these medical illustrations, you are taking a major step toward protecting your mobility.
Conclusion: Empowering Your Joint Health Journey
Navigating the world of arthritis can feel overwhelming, but knowledge is the most powerful tool in your arsenal. Whether you are dealing with the sharp, sudden intensity of Gout or the slow, persistent ache of Osteoarthritis, understanding the “why” behind the pain allows you to take targeted action. Remember that Gout is an internal chemical battle that requires metabolic management, while Osteoarthritis is a structural challenge that requires physical support and protective habits.
By focusing on the right diet, maintaining an active lifestyle, and working closely with healthcare professionals, you can manage these conditions effectively. Do not let joint pain sideline your passions. Take a look at your symptoms, consult the experts, and start building a plan that keeps you moving comfortably for years to come. Your joints do a lot for you, and with the right care, you can return the favor.